
Why real-world materials and user testing is critical to medical device success
August 2022
by Sarah Knight, Head of Healthcare at 42T
Real-world data and testing, risk management, and post market surveillance can make or break a product
A year ago, Philips Respironics initiated a voluntary recall of more than 5 million respiratory devices due to potential health risks related to the sound abatement foam breaking down over time - potentially releasing particulates and degradation chemicals into the patient’s airways.
This event illustrates the importance of understanding how your device will be used during all elements of its use cycle – and also the value of post market surveillance in catching patient safety issues. Together, these can be used to ensure the development team know what conditions a device will be subjected to, and test appropriately.

In a recent update, Philips implied that degradation could have been caused or exacerbated by the use of ozone cleaning. Whilst ozone cleaning was not indicated in the instructions for use, the investigation uncovered that significant numbers of devices were subjected to this cleaning method by users. These devices were fourteen times more likely to have visible foam degradation.
This example shows us the importance of gaining a deep knowledge of how your device may be used - including by different users, in various settings and locations. Plus, it illustrates that thorough material testing is essential to understand, and design out potential product vulnerabilities and patient risks.
This applies for all kinds of medical devices – from medical electrical equipment, to implants and wearables.
Understand the use process
In the case of medical implants, everyone is very much aware that unintended material deterioration can be dangerous, such as the wear of metal-on-metal hip implants. But it’s not only the environment inside the patient’s body that engineers need to understand. They also need to be aware of how surgeons interact with the device prior to or during the implantation procedure, and what substances it might contact.
For example, just because an implant or tool is supplied sterile doesn’t mean that it will never encounter cleaning solutions. Engineers at 42 Technology (42T) have previously been involved in a focus group study with surgeons and other stakeholders, during the development of a new coated implant.
An important learning was that with the existing implant, some surgeons used antiseptic solutions to clean the implant or the cavity immediately prior to implantation.
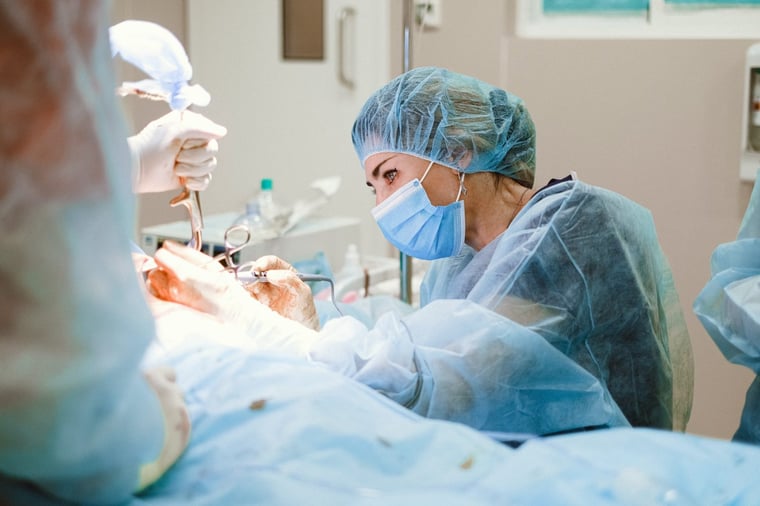
In fact, the use of substances like Betadine (Povidone-iodine) is common practice, thought to disrupt biofilm formation and reduce the risk of complications such as surgical site infections. Also, in the case that an implant does become infected, solutions containing antiseptics or antibiotics may be used to irrigate the infected cavity prior to reimplantation.
The development team was able to investigate the compatibility of the new coating with a range of commonly used solutions to inform the development and risk management processes.
Test materials thoroughly
Devices used outside of a healthcare setting can be subject to a wide range of conditions. For example, in the field of wearables, products are used in all kinds of everyday environments by lay users. Companies such as Nanowear, Bloomer Tech and KYMIRA are developing ‘smart garment’ devices that can measure the wearer’s lung volume, take an electrocardiogram, or deliver infrared therapy.
The potential for unobtrusive, always-on devices to change how conditions are monitored or treated is incredibly exciting. Understanding how the devices will be used (and misused) in the field is key to ensuring patient safety and acceptable product life.
In a recent project at 42T, it was discovered that domestic laundry cycles can subject such garments to surprisingly extreme conditions. During testing, engineers added laundry products at minimum and maximum dosage amounts that could be anticipated for users who may be trying to follow recommendations on the packaging. These included detergents, fabric care products, and common home remedies such as white vinegar.

Then they ran a range of wash cycles while measuring conditions in the wash mixture. Across these scenarios, the pH of the wash ranged between 4 and 10. For users who ignore the packaging, the pH may be even more extreme. This example shows that it’s important to test the limits of what you can expect users to do, not just check your device is compatible with an ‘average’ wash.
Manage risk
To understand the hazards that exist, the development team needs to understand the use process in order to identify what conditions or chemicals the device could be exposed to. To estimate and evaluate the risk, good material compatibility data is invaluable.
Gathering these insights and evidence early means that the development team can implement appropriate controls based on the hierarchy presented in ISO 14971. This describes a priority order for the use of risk control options:
- Inherently safe design and manufacture
- Protective measures e.g. a guard or filter
- Information for safety or training
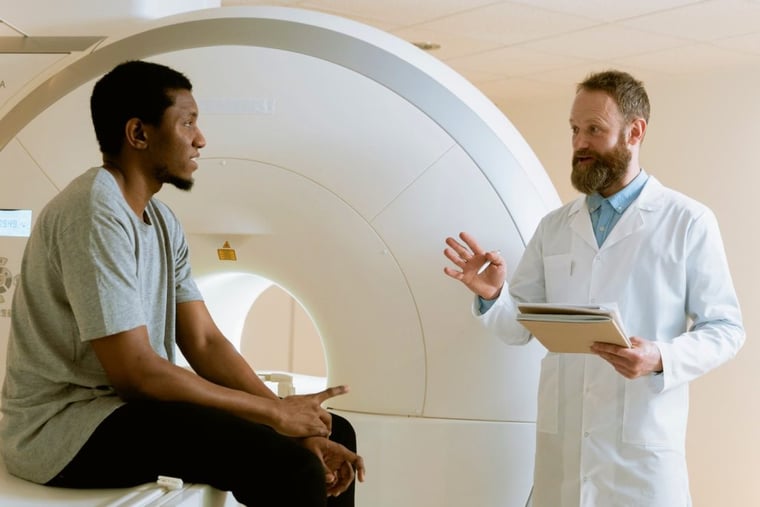
We can now see that had Philips known the extent of the risk of ozone cleaning, they would not have relied on merely providing cleaning information in the instructions. In fact, in September 2021 Philips began replacing the foam in recalled devices with a new material – following the principle of inherent safety by design.
Post-market surveillance
Understanding the use case and testing does not necessarily stop when a device reaches the market. Critical aspects of use may change over time – particularly over the lifetime of a costly piece of hospital equipment such as a ventilator. Perhaps new cleaning products or accessories become available, or older ones are discontinued.
The user may change: perhaps national shortages of a particular specialism means that providers shift certain tasks to more junior staff or a different member of the multidisciplinary team. Post-market surveillance should be designed to help you understand how devices continue to be used, recognise any changes, and take action to understand their impact early.
Real-world data is key
The common theme here is that we can’t rely only on theoretical or idealised information. User interviews and observations will almost always uncover new insights into user behaviour – ways that users in the field might deviate from what’s considered ‘normal’ to a designer in the office.

Even if detailed chemical compatibility data exists for the particular material grade in consideration, it is very unlikely to cover the full range of conditions that a device is reasonably anticipated to encounter.
Early in the development process, conceptual designs might be based on the expected user process and textbook compatibility data. But testing these out as soon as possible in the real world is not just best practice – it can be critical.

If you would like to find out more, please contact Sarah:
answers@42T.com | +44 (0)1480 302700 | Sarah Knight | LinkedIn
Sarah is a chartered engineer (IMechE). She holds an honours degree in Biomedical Engineering and a Master’s degree in Mechanical Engineering from Cambridge University.
She is also an experienced project manager with particular expertise in medical device development and has guided products through all stages of development from innovative concepts to detailed design, regulatory approval, and troubleshooting in manufacture.
Share this article:
Related Articles
Healthcare & Life Sciences
How to rescue medical devices from component problems


Healthcare & Life Sciences
Innovations and future tech spotted at this year's MEDICA event

What will you ask us today?
We believe in asking the right questions to drive innovation; when we know the right questions, we generate the ideas to answer them.

